TFRI funding for researchers at the Centre for Lymphoid Cancer (BC Cancer Agency) has resulted in the discovery that subtype-specific alterations in a driver gene for non-Hodgkin lymphoma (BCL2) is strongly associated with poor patient outcomes after treatment.
The work by Drs. David Scott, Randy Gascoyne, Joseph Connors, and Christian Steidl was published in Blood (May 2017). Diffuse large B-cell lymphoma (DLBLC) is the most common type of non-Hodgkin lymphoma, predominantly affecting people in their mid-60s. BCL2 and MYC are critical driver genes for the disease and play key roles in in normal B-cell differentiation and tumourigenesis.
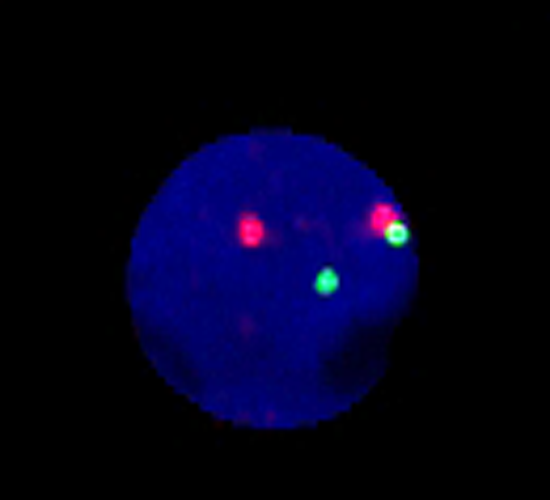
Genetic alterations in both genes were profiled in the present study via next-generation sequencing and high-resolution SNP array in 347 de novo DLBCL patients that had already been treated with R-CHOP, the standard chemotherapy treatment for this disease. The team discovered the clinical impact of genetic aberrations in DLBLC needs to be placed in the context of the cell-of-origin molecular subtype and, when this is done, subtype-specific alterations in BCL2 are revealed as being strongly associated with poor outcomes post treatment.
Further, this work showed that the incidence of MYC/BCL2 genetic alterations and their clinical significance were mainly dependent on cell-of-origin (COO) subtypes. There are two main subtypes of DLBLC based on COO, activated B-cell-like (ABC) subtype and the germinal center B-cell-like (GCB) subtype, both of which have different biology and clinical behaviour. In ABC and GCB subtypes, gain of BCL2 and translocation of BCL2 respectively often led to poor outcomes. The results suggest that COO subtype-specific biomarkers based on these BCL2 genetic alterations can be effectively used to risk-stratify patients with DLBCL treated with immunochemotherapy.
This paper highlights the value of examining clinical correlates in large homogeneously treated population registry-based cohorts. The finding that BCL2 dysregulation is a common feature of patients with inferior survival will prioritize examination of therapeutic approaches that target BCL2, and hopefully result in better patient outcomes in the future.
Study: Genetic profiling of MYC and BCL2 in diffuse large B-cell lymphoma determines cell-of-origin–specific clinical impact
Authors: Daisuke Ennishi, Anja Mottok, Susana Ben-Neriah, Hennady P. Shulha, Pedro Farinha, Fong Chun Chan, Barbara Meissner, Merrill Boyle, Christoffer Hother, Robert Kridel, Daniel Lai, Saeed Saberi, Ali Bashashati, Sohrab P. Shah, Ryan D. Morin, Marco A. Marra, Kerry J. Savage, Laurie H. Sehn, Christian Steidl, Joseph M. Connors, Randy D. Gascoyne, and David W. Scott.
Funding: This study was supported by a Program Project Grant from the Terry Fox Research Institute (Grant No. 1023 to R.D.G.)
TFRI LINKS, Summer 2017