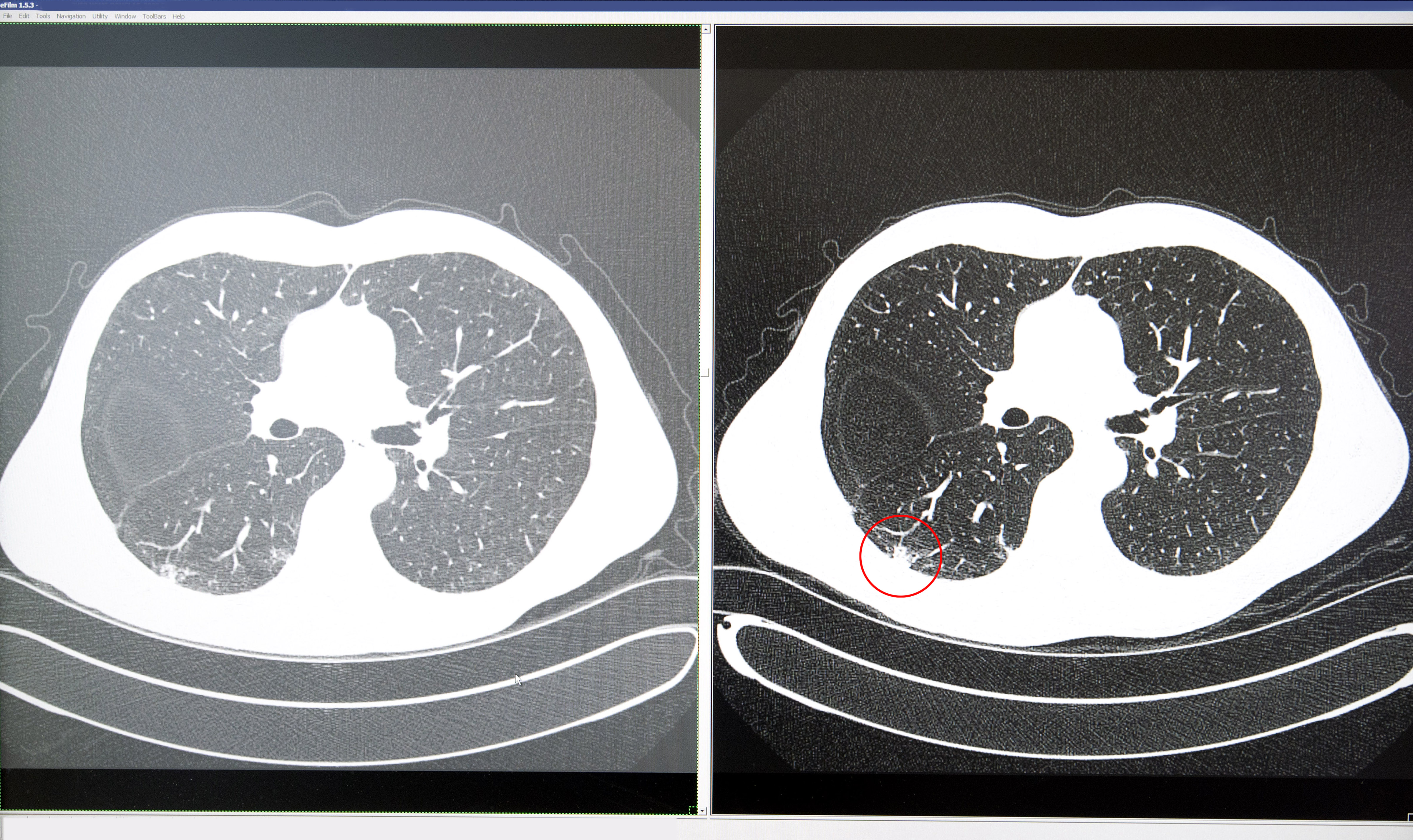
New research from a TFRI-funded team suggests screening for lung cancer could save money – and lives – especially if it also identifies other tobacco-related conditions in high-risk individuals.
This study was published in the Journal of Thoracic Oncology (May 2017), and suggests combining CT screening for multiple conditions with efforts to stop smoking and manage the treatment of non-cancer heart and lung disease could make screening even more cost-effective.
Lung cancer is the most common cause of cancer death around the world, with 1.6 million deaths and 1.8 million new cases a year. The five-year for survival rate for patients is currently less than 18 per cent, but if caught early enough the disease can be cured for 70 per cent of cases.
Lead author Dr. Sonya Cressman (The Canadian Centre for Applied Research in Cancer Control/BC Cancer Agency) says researchers need to think about how to manage lung cancer while focusing on economically viable strategies such as prevention and screening.
“Screening those at a high-risk gives us the chance to prevent and treat a range of tobacco-related illnesses, and could also offer access to care for individuals who could be otherwise stigmatized or segregated from receiving treatment,” she said.
Patient data from two major screening trials was examined: The National Lung Cancer Screening Trial (NLST) and the TFRI Pan-Canadian Early Detection of Lung Cancer Study (PanCan). An economic model was built to simulate the costs and benefits of introducing lung cancer screening programs for high-risk people, or those who had a two per cent or higher chance of developing lung cancer within six years.
Using this data, the team determined the overall cost-effectiveness of the program could be substantially increased if the health of the people being screened were to improve. Focusing on high-risk people could reduce the number of individuals who need to be screened by more than 80 per cent, the study suggests.
The cost of screening was calculated to be $20,724 per year of life saved, a number considered to be cost-effective compared to the benchmark of $100,000 that is often paid for other cancer interventions in national healthcare.
“Working with this team of investigators has driven the success of the study,” said Cressman. “The project arose from a strong multidisciplinary collaboration bringing together experts from across Canada who are passionate about public health and willing to invest their protected time in finding ways to optimize the way lung cancer care is delivered.”
This research was predominantly funded by the Terry Fox Research Institute, the Partnership Against Cancer, and the Canadian Centre for Applied Research in Cancer Control.
Click here to learn more about TFRI’s Pan-Canadian Early Lung Cancer Detection Study.

The study's lead author Sonya Cressman.